Observation of the Natural Evolution of Insomnia in the U.S. population
First created | 01/12/1999
Last edited |
- Ohayon MM. Observation of the Natural Evolution of Insomnia in the American General Population Cohort. Sleep Med Clin 2009; 4:87-92. Free PMC Article
Insomnia symptoms are the most frequent sleep disturbances affecting about one third of the general population (Ohayon, 2001).
Factors associated with insomnia symptoms are numerous; mental disorders and organic diseases being among the most frequent observed associations.
Nonetheless, epidemiological studies that have examined these associations remain uncommon partly because of the complexity of assessing mental disorders in the general population and the costs involved in doing lengthy interviews.
Longitudinal studies that have examined the evolution of insomnia symptoms are nearly non-existent and limited in terms of studied associations.
Existing studies that examined the associations between insomnia and mental disorders are briefly reviewed along with consequences of insomnia.
New data on a longitudinal study we performed in our center are also presented.
ASSOCIATION MENTAL DISORDERS AND INSOMNIA
Cross-sectional studies have shown that subjects with insomnia exhibit symptoms of depression in 40% to 60% of the cases (Mellinger et al., 1985; Henderson et al., 1995; Foley et al.,1995; Ohayon et al., 1998).
Clinical depression was observed in 10% to 25% of insomnia cases (Ohayon et al., 1997, 2000;2003; Maggi et al., 1998; Taylor et al., 2005).
Anxiety is more common: subjects with insomnia have anxiety disorders in 20% to 30% of cases (Ohayon et al., 1997, 2000;2003; Maggi et al., 1998; Taylor et al., 2005).
Diagnostic distribution of subjects with insomnia is displayed in figure 1.
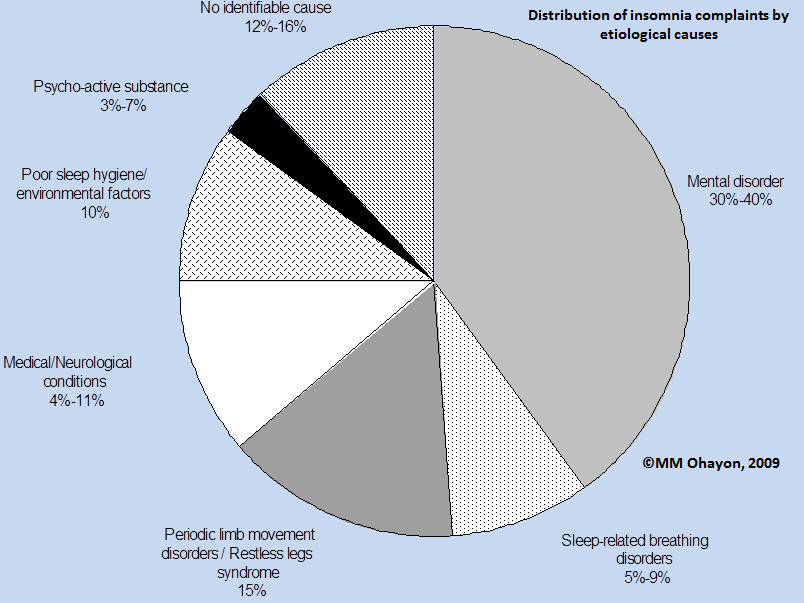
As seen, mental disorders are observed in 30% to 40% of insomnia complaints.
Sleep-related breathing disorders such as obstructive sleep apnea syndrome or hypoventilation account for 5% to 9% of insomnia complaints (Ohayon, 2001; Buysse et al., 1994; Ohayon and Roth, 2001; Jacobs et al., 1988).
Periodic limb movement disorders and/or restless legs syndrome are found in about 15% of individuals with insomnia complaints (Buysse et al., 1994; Ohayon and Roth, 2001; Edinger et al., 1996; Ohayon and Roth, 2002).
Medical or neurological conditions are observed in 4% to 11% of insomnia complaints (Ohayon, 2001; Buysse et al., 1994; Jacobs et al., 1988).
Poor sleep hygiene or environmental factors account for about 10% of insomnia complaints, and substance-induced for 3% to 7% (Ohayon, 2001).
Multiple associated conditions can be observed in as many as 30% of individuals with insomnia complaints (Ohayon, 2006).
In summary, the association between insomnia, depression and anxiety has been highlighted in numerous studies. However, little is known about factors that may influence this relationship. Consequently, a better control over other predictors of mental disorders such as obesity or chronic pain might offer a clearer picture of the association between mental disorder and insomnia.
From longitudinal studies, we know that insomnia at point 1 predicts depression at point 2 (Ford & Kamerow, 1989; Breslau et al., 1996; Weissman et al., 1997; Roberts et al., 2000; Jansson, 2006). Furthermore, the persistence of insomnia (present in both evaluation) is a stronger predictor of depression at point 2 (Ford & Kamerow, 1989; Roberts et al., 2000; Perlis et al., 2006).
Most longitudinal studies have analyzed the association insomnia-mental disorders as an unidimensional phenomenon while multi-dimensional models would be more appropriate. It remains to know in what extend insomnia a precursor rather than a cause of mental disorder.
CONSEQUENCES OF INSOMNIA
Consequences of insomnia can be found at several levels:
- Development of a medical condition;
- Development of a mental disorder;
- Repercussions on daytime functioning;
- Road, work, domestic accidents.
DEVELOPMENT OF A MEDICAL CONDITION
Several studies attempted to determine whether insomnia may be responsible of cardiovascular accidents.
However the results are inconclusive. One study found that individuals with insomnia had a 3.1 relative risk of developing cardiovascular accident (Mallon et al., 2002) while other studies found no causality between insomnia and risk of developing a cardio-vascular disease and another study found greater likelihood of developing insomnia after a cardio-vascular accident (Foley et al., 1999).
DEVELOPMENT OF A MENTAL DISORDER
A study (Ohayon and Roth, 2003) examining the time sequence between insomnia and mood and anxiety disorders, reported that insomnia was present in 70% of cases with mood disorders and that it preceded the apparition of the mood disorders in nearly half of cases (figure 2a).

Insomnia was found in one third of cases with anxiety disorders. Insomnia symptoms preceded the anxiety disorders in about one fifth of cases (figure 2b).

REPERCUSSIONS ON DAYTIME FUNCTIONING
Repercussions on daytime functioning are present in 20% to 60% of individuals with insomnia (Ohayon et al., 1997; 2001; Hetta et al., 1999; Hoffmann et al., 1999; Leger et al., 2000).
Individuals who poorly sleep at least 3 nights per week, are dissatisfied with their sleep, are unrested upon awakening and have hyperarousal in bed are the most likely to have repercussions on daytime functioning (Ohayon et al. 1997, 2001).
ROAD, OCCUPATIONAL AND DOMESTIC ACCIDENTS
Road accidents are 2 to 3 times more frequent in drivers dissatisfied with their sleep (Ohayon et al., 2001, 2002).
They are also more frequent in short sleepers (< 5 hours) (Connor et al., 2002; McCartt et al., 1996).
In elderly, insomnia was associated with increased risk of hip fracture (Fitzpatrick et al., 2001), and falls (Brassington et al., 2000; Mendez Rubio et al., 1997).
Another study found a relative risk of 1.9 for fatal occupational accidents in individuals with difficulty in sleeping (Akerstedt et al., 2002).
ASSOCIATIONS BETWEEN PAIN, MENTAL DISORDERS, ORGANIC DISEASES AND INSOMNIA SYMPTOMS
The Venn's diagram in figure 3 shows the interaction between insomnia symptoms, mental disorders, organic diseases and dyssomnia diagnoses (insomnia disorder, obstructive sleep apnea, restless legs syndrome, circadian rhythm disorders; hypersomnia; narcolepsy) (M. Ohayon, personal data on the European population).
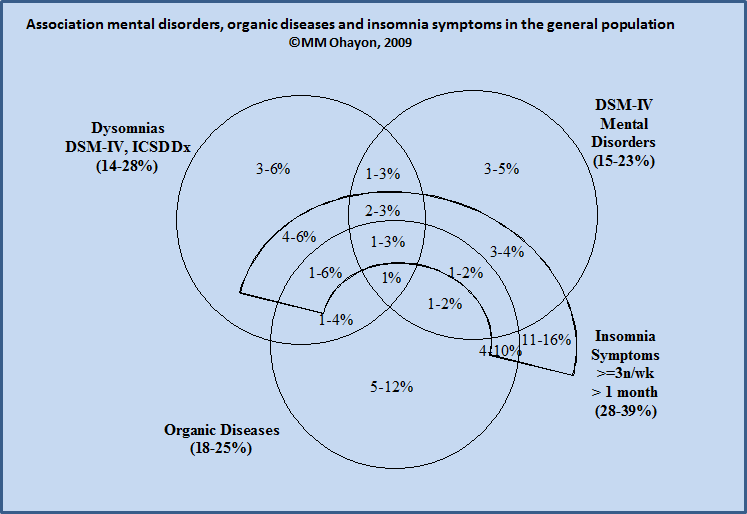
As seen, insomnia symptoms rarely occur alone. In half cases a concurrent organic disease is observed; in a third of cases a mental disorder is present and in 1 on 10 organic disease and mental disorder are present.
In nearly 70% of cases, mental disorders are concomitant with organic diseases and/or other dyssomnias.
More than 50% of organic diseases are accompanied with mental disorders and/or other dyssomnias.
The Venn's diagram in figure 4 shows the associations between chronic pain, mental disorders, organic diseases and insomnia symptoms in the American general population (M. Ohayon, personal data).
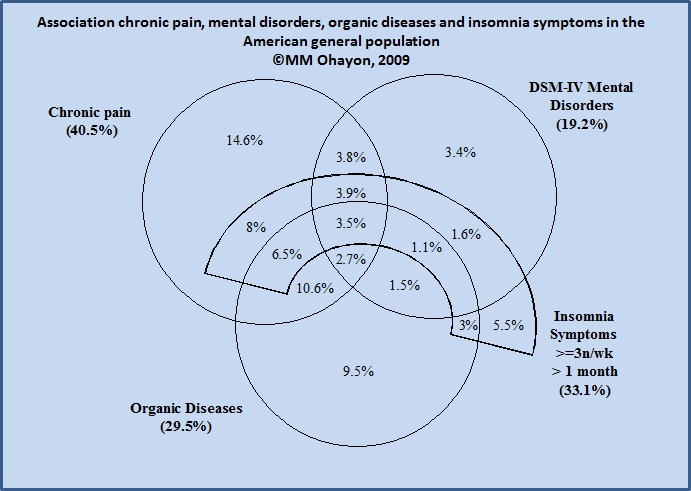
As seen, as many as 66.8% of insomnia symptoms are associated with chronic pain.
Similarly, 72% of subjects with mental disorders and 79% of subjects with organic disease also have chronic pain.
EVOLUTION OF INSOMNIA AND MENTAL DISORDERS
A longitudinal study of a representative sample of the Californian general population was undertaken in 2005 and 2006 in our Center.
The baseline sample included 3,249 adults from the general population interviewed between 2002 and 2003. At the end of the interview, they were asked if they were willing to be interviewed again in the future; 2,729 agreed to be part of the longitudinal survey.
The follow-up was done 3 years after the initial interview.
A total of 1,957 individuals of the baseline sample was reached. Among participants lost to follow-up:
- 17 had died;
- 41 were seriously ill or hospitalized;
- 379 numbers were disconnected;
- 132 refused to participate and
- 203 numbers were attributed to a new household.
EVOLUTION OF INSOMNIA
At baseline, 42.1% of the 1,957 individuals that participated in the follow-up had insomnia symptoms at least 3 nights per week for at least one month.
Three years later, 72.2% of them still had insomnia symptoms.
On the other hand, among those without insomnia symptoms at baseline, 15.5% developed insomnia symptoms (Figure 5).
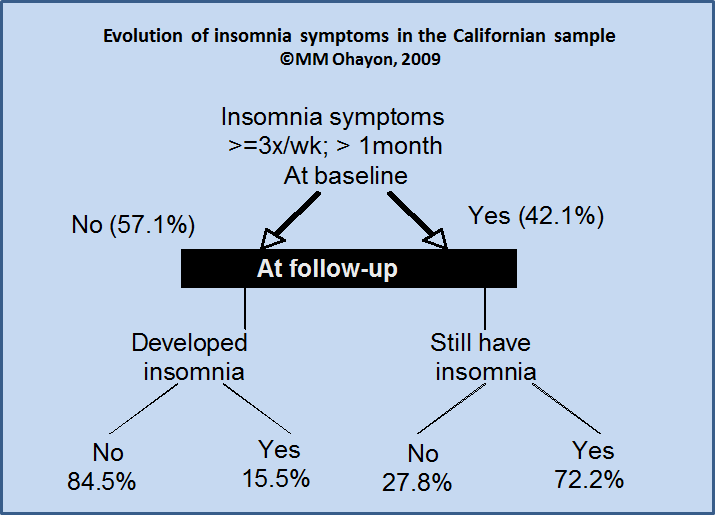
PRE-EXISTING CHRONIC PAIN AND MENTAL DISORDERS FOR DEVELOPMENT OF INSOMNIA
We examined whether pre-existing chronic pain (pain lasting for at least 3 months) and mental disorders (without insomnia symptoms) were predictors for the development of insomnia.
After adjusting for age, gender and race, we found that individuals with a major depressive disorder had a relative risk of 3.8 of developing insomnia at 3-year follow-up. Among individuals with anxiety disorder, the relative risk of developing insomnia was 2.6 and the relative risk of developing insomnia was 1.8 among individuals with chronic pain.
INSOMNIA AS A PREDICTOR FOR THE DEVELOPMENT OF CHRONIC PAIN AND MENTAL DISORDERS
We also examined whether insomnia symptoms were predictors for the development of chronic pain and mental disorders.
Subjects with insomnia symptoms but without major depressive disorder at baseline had a relative risk of 2.1 of developing a major depressive disorder at 3-year follow-up.
Subjects with insomnia symptoms but without anxiety disorder at baseline had a relative risk of 1.9 of developing an anxiety disorder at 3-year follow-up.
Presence of insomnia at baseline was not significantly associated with chronic pain at 3-year follow-up.
CONCLUSIONS
Existing cross-sectional epidemiological studies tend to examine associations between insomnia and mental disorders only in a bi-dimensional way.
However, many other factors related to both insomnia and mental disorders might have confounding effects on this association.
One of the possible consequences would be an amplification effect on odds ratios when no control is exerted on possible confounding variables.
We have shown in the two Venn's diagrams that insomnia symptoms and mental disorders are also often associated with several organic diseases and chronic pain.
In our longitudinal study, we have demonstrated that insomnia, psychiatric disorders, organic diseases and pain are closely interrelated.
Major depressive disorder at baseline was the strongest predictor of developing insomnia.
Insomnia at baseline was associated with 3 times the risk of developing a major depressive disorder and anxiety at 3-year follow-up.
Further analyses on the effects of confounding variables will offer a clearer picture on how insomnia is closely related to the development of a psychiatric disorder.
REFERENCES
- Akerstedt T, Fredlund P, Gillberg M, Jansson B. A prospective study of fatal occupational accidents - relationship to sleeping difficulties and occupational factors. J Sleep Res. 2002;11:69-71.
- Brassington GS, King AC, Bliwise DL. Sleep problems as a risk factor for falls in a sample of community-dwelling adults aged 64-99 years. J Am Geriatr Soc. 2000;48:1234-1240.
- Breslau N, Roth T, Rosenthal L, Andreski, P. Sleep disturbance and psychiatric disorders: a longitudinal epidemiological study of young adults. Biol Psychiatry 1996; 39:411-418.
- Buysse DJ, Reynold CF, Hauri P, Roth T, Stepanski E, Thorpy MJ, Bixler E, Kales A, Manfredi, R, Vgontzas A, Stapf BS, Houck PR, Kupfer DJ. Diagnostic concordance for DSM-IV disorders: a report from the APA/NIMH DSM-IV field trial. Am J Psychiatry 1994; 151:1351-1360.
- Connor J, Norton R, Ameratunga S, Robinson E, Civil I, Dunn R, Bailey J, Jackson R. Driver sleepiness and risk of serious injury to car occupants: population based case control study. BMJ. 2002;324:1125.
- Edinger JD, Fins AI, Goeke JM, McMillan DK, Gersh TL, Krystal AD, McCall WV. The empirical identification of insomnia subtypes: a cluster analytic approach. Sleep. 1996;19:398-411.
- Fitzpatrick P, Kirke PN, Daly L, Van Rooij I, Dinn E, Burke H, Heneghan J, Bourke G, Masterson J. Predictors of first hip fracture and mortality post fracture in older women. Ir J Med Sci. 2001;170:49-53.
- Foley DJ, Monjan A, Simonsick EM, Wallace RB, Blazer DG. Incidence and remission of insomnia among elderly adults: an epidemiologic study of 6,800 persons over three years. Sleep 1999;22 Suppl 2:S366-S372.
- Foley DJ, Monjan AA, Brown SL, Simonsick EM, Wallace RB, Blazer DG. Sleep complaints among elderly persons: an epidemiologic study of three communites. Sleep 1995; 18:425-432.
- Ford DE, Kamerow DB. Epidemiologic study of sleep disturbances and psychiatric disorders. An opportunity for prevention? JAMA, 1989; 262:1479-1484.
- Henderson S, Jorm AF, Scott LR, Mackinnon AJ, Christensen H, Korten AE. Insomnia in the elderly: its prevalence and correlates in the general population. Med J Aust 1995; 162:22-24.
- Hetta J, Broman JE, Mallon L. Evaluation of severe insomnia in the general population-implications for the management of insomnia: insomnia, quality of life and healthcare consumption in Sweden. J Psychopharmacol 1999;13(4 Suppl 1):S35-S36.
- Hoffmann G. Evaluation of severe insomnia in the general population--implications for the management of insomnia: focus on results from Belgium. J Psychopharmacol 1999;13(4 Suppl 1):S31-S32.
- Jacobs EA, Reynolds CF 3rd, Kupfer DJ, Lovin PA, Ehrenpreis AB. The role of polysomnography in the differential diagnosis of chronic insomnia. Am J Psychiatry. 1988;145:346-349.
- Jansson M, Linton SJ. The development of insomnia within the first year: a focus on worry. Br J Health Psychol. 2006;11(Pt 3):501-511.
- Leger D, Guilleminault C, Dreyfus JP, Delahaye C, Paillard M. Prevalence of insomnia in a survey of 12,778 adults in France. J Sleep Res 2000;9:35-42.
- Maggi S, Langlois JA, Minicuci N, Grigoletto F, Pavan M, Foley DJ, Enzi G. Sleep complaints in community-dwelling older persons: prevalence, associated factors, and reported causes. J Am Geriatr Soc 1998;46:161-168.
- Mallon L, Broman JE, Hetta J. Sleep complaints predict coronary artery disease mortality in males: a 12-year follow-up study of a middle-aged Swedish population. J Intern Med 2002;251:207-216.
- McCartt AT, Ribner SA, Pack AI, Hammer MC. The scope and nature of the drowsy driving problem in New York State. Accid Anal Prev. 1996;28:511-517.
- Mellinger GD, Balter MB, Uhlenhuth EH. Insomnia and its treatment: Prevalence and correlates. Arch Gen Psychiatry 1985; 42: 225-232.
- Méndez Rubio JI, Zunzunegui MV, Béland F. Méndez Rubio JI, Zunzunegui MV, Béland F. The prevalence of and factors associated with falls in older persons living in the community (in Spanish). Med Clin (Barc). 1997;108:128-132.
- Ohayon MM, Caulet M, Lemoine P. Comorbidity of mental and insomnia disorders in the general population. Compr Psychiatry 1998;39:185-197.
- Ohayon MM, Roth T. Place of chronic insomnia in the course of depressive and anxiety disorders. J Psychiatr Res. 2003;37:9-15.
- Ohayon MM, Roth T. Prevalence of restless legs syndrome and periodic limb movement disorder in the general population. J Psychosom Res 2002; 53:547-554.
- Ohayon MM, Roth T. What are the Contributing factors for Insomnia in the General Population? J Psychosom Res 2001;51:745-755.
- Ohayon MM, Shapiro CM, Kennedy SH. Differentiating DSM-IV Anxiety and Depressive Disorders in the general population: comorbidity and treatment consequences. Can J Psychiatry 2000; 45:166-172.
- Ohayon MM, Smirne S. Prevalence and consequences of insomnia disorders in the general population of Italy. Sleep Medicine 2002; 3:115-120.
- Ohayon MM. Epidemiology of insomnia: what we know and what we still need to learn. Sleep Med Rev 2002; 6:97-111.
- Ohayon MM. Interlacing sleep, pain, mental disorders and organic diseases. J Psychiatr Res. 2006;40:677-679.
- Ohayon MM. Prevalence of DSM-IV diagnostic criteria of insomnia: Distinguishing between insomnia related to mental disorders from sleep disorders. J Psychiatr Res 1997; 31: 333-346.
- Perlis ML, Smith LJ, Lyness JM, Matteson SR, Pigeon WR, Jungquist CR, Tu X. Insomnia as a risk factor for onset of depression in the elderly. Behav Sleep Med. 2006;4:104-113.
- Roberts RE, Shema SJ, Kaplan GA, Strawbridge WJ. Sleep complaints and depression in an aging cohort: A prospective perspective. Am J Psychiatry 2000;157:81-88.
- Taylor DJ, Lichstein KL, Durrence HH, Reidel BW, Bush AJ. Epidemiology of insomnia, depression, and anxiety. Sleep. 2005;28:1457-1464.
- Weissman MM, Bland RC, Canino GJ, Faravelli C, Greenwald S, Hwu HG, Joyce PR, Karam EG, Lee CK, Lellouch J, Lepine JP, Newman SC, Rubio-Stipec M, Wells JE, Wickramaratne PJ, Wittchen H, Yeh EK. Cross-national epidemiology of major depression and bipolar disorder. JAMA 1996;276:293-299.
Ohayon MM. Observation of the Natural Evolution of Insomnia in the American General Population Cohort. Sleep Med Clin 2009; 4:87-92. Free PMC Article
